…and Paul’s not even a physician or physical therapist. But he’s a smart guy, writer, and former massage therapist. Click for his article on patello-femoral pain syndrome if interested. I paid about $20 USD for the full article, and it was well worth it. Full disclosure: I don’t know Paul and earn no commission or other compensation for this endorsement.
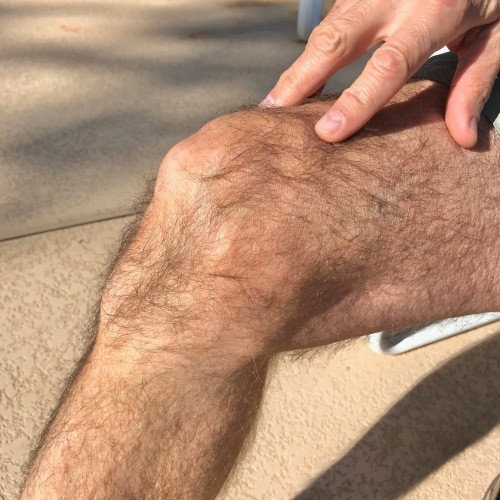
Photo credit: Steven Paul Parker II
The key to my cure was probably radical rest, or what Paul calls profound rest.
If you have PFPS, I hope you find something useful here.
Regular readers here know I’m a huge proponent of exercise. Unfortunately, exercise can be risky. You can injure yourself. I did that a few years ago when I was getting in shape to climb Humphreys Peak. I accelerated my training program too rapidly and developed patell0-femoral pain syndrome (PFPS).
This is how my right knee felt in 2017:
I’ve developed over the last month some bothersome pain in my right knee. It’s not interfered much with my actual hiking, but I pay for it over the subsequent day or two. I’m starting to think this may put the kibosh on my Humphries Peak trek next month.
The pain is mostly anterior (front part of the knee) and is most noticeable after I’ve been sitting for a while with the bent knee, then get up to walk. The pain improves greatly after walking for a minute or less. It also hurts a bit when I step up on something using my right leg. If I sit with my knee straight (in full extension), it doesn’t hurt when I get up. The joint is neither unusually warm nor swollen. Ibuprofen doesn’t seem to help it.
That episode resolved after I stopped hiking for 3-4 months. But in 2018 I had recurrence of similar pains in my left knee, with no clear precipitant this time. I continued my usual weight-training program and expected another spontaneous resolution. Six months passed…no improvement. That’s when I found Paul Ingraham’s article.
By the way, I’m the one who diagnosed my PFPS. It’s been said that a doctor who diagnoses and treats himself has a fool for a patient. He can’t be adequately objective.
Alternative diagnoses would include patello-femoral osteoarthritis and degenerative meniscus, due to my age (over 60). Diagnosis of the osteoarthritis could be facilitated by knee X-rays: weight-bearing posterior-anterior imaging, weight-bearing lateral view, and sunrise view.
This was my treatment plan for PFPS in early Feb 2019, based on Paul Ingraham’s recommendations. Paul explains how to do various specific exercises below in his article.
- Avoid all activities that stress the patella-femoral joint or aggravate pain for at least two weeks, if not longer (2–3 months). Paul calls it “profound rest.” I started this Feb 17. No knee-loading exercise (e.g., leg presses, any kind of squat, deep knee bends) until pain is truly in remission from rest. I quit my usual squats, Bulgarian split-squats, and single-leg Romanian deadlifts.
- Consider Motrin (ibuprofen) 400-600 mg three times daily for two weeks (I did 600 mg 3x/day) but usually no help
- Consider cold-packs (10–20 mins) when it flares up but usually no help. (I never did this because I couldn’t find my WalMart cold-pack.)
- Find a substitute for the squats? E.g., stationary bike? No bike for now: too much stress on patello-femoral joint at this time
- Paul’s not big on stretching (quadriceps and hamstring stretches routinely recommended by others). I didn’t stretch.
- While recovering, keep leg straight most of the time, even when sitting. Sit less. (I didn’t sit less but did make a huge effort to keep my affected led fully extended, or at least not bent more that 20 degrees at any time. This necessitated sitting on the edge of my seat at work, and/or lowering the height of the seat. At home relaxing, I’d keep my leg fully extended. I think this was extremely important for my healing. I considered getting a standing desk for home or work but didn’t.)
- Start with exercises that keep knees straight. Exercise both lower extremities. As condition improves, can start to add other exercises, very slowly, that allow bent knees. Single-leg RDLs may be a good start (started in Sept 2019). Restart squats, deep knee bends, and leg presses (cycling?) only very late into recovery. Rehab must progress VERY SLOWLY. If an exercise causes more knee pain, back off and work the hips first. Exercise 2–3 times/week. Walking on the flat in moderation is usually OK. Strengthening hip abductors may be helpful.
- Hamstring curls via machine or therabands. Curl to 60 degrees, not 120. (I curled to 90 degrees using therabands).
- Quadricep setting. (I didn’t do this. Straight-leg raises on your back seem to be similar, which I did.)
- Straight-leg raises, on back and side-lying. (Done: 3 sets of 10 reps each side.)
- Clam shells. (Done: 3 sets of 10 reps each side.)
- Knee lifts? (don’t know what that is; not done).
- Consider the following although not from Paul: Hip abductor strengthening: “monster walks” (lateral steps with elastic band around (just proximal to) knees: 1 min x 3 sets. Hip hikes (what’s this?): 2 sets of 20 reps each side.
- Consider the following although not from Paul: Quad strengthening: terminal knee extensions with elastic band, 3 sets of 15 reps; leg presses?; semi squat, 3 sets of 10 reps (also recumbent bike?). Also consider stork stance TKE (terminal knee extensions) as alternative to standard TKE.
- Paul likes trekking poles for hikers. (I’ve been using these for years; Leki brand.)
- Not from Paul: Home physical therapy for six weeks
- Not from Paul: Turkish get-ups now or later? Much further into recovery!
Update of Progress on April 4, 2019:
Knee definitely feeling better, probably due to profound rest as above. On Feb 23, I aggravated knee mildly by sledding in snow with Paul in Care Free – no regrets! Around Feb 26, Sunny got me started on Platinum’s Ortho-Chon Plus, 3 caps twice daily. Per 3 caps: glucosamine sulfate 800 mg, turmeric 380 mg, methylsulfonylmethane 350 mg, berberine HCL 145 mg, Boswellia serrata extract 140 mg, hyaluronic acid 50 mg, cat’s claw 10 mg, total cetylated fatty acids 3 mg. Not sure if these did any good at all; I’m skeptical. Started feeling less pain around Feb 29.
I am not healed or in remission yet. Doing hip exercises twice or once/wk with Therabands: clamshells, straight leg raises, side-lying straight leg raises, hamstring curls.
I had to put hip exercises on hold temporarily on March 28 due to a right low back muscle strain either from the exercises or weed pulling.
Update on Nov 25, 2019:
The PFPS is in remission and has been since July or so. For the last couple months I’ve been doing single-leg Romanian deadlifts and “walking” on elliptical-type aerobic machines at Anytime Fitness—some machines also work the upper limbs, others don’t—which are very easy on my knees. Avoiding treadmill since I have a palpable click in one knee, and treadmill aggravates my degenerative joint disease (DJD in both knees but predominantly left knee).
Next step is to slowly re-introduce exercises that load the knees (particularly the patell0-femoral joint). This is scary but must be done. My quads have atrophied somewhat. Squats? Lunges? Bulgarian split squats?
Steve Parker, M.D.

Click the pic to purchase at Amazon.com. E-book versions also available at Smashwords. com





















