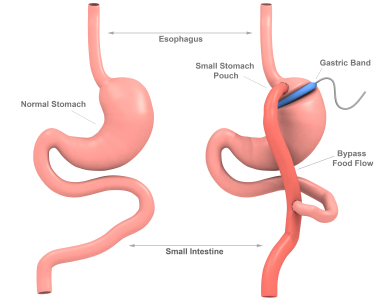
The only picture of stomach I have
When you eat a meal, your stomach holds it there for a while then gradually releases contents into the duodenum, the first part of the small intestine. The stomach makes those releases by contraction of muscles in the wall of the stomach. Those muscles are under control of the autonomic nervous system. In some folks with diabetes, the nerves controlling the stomach muscles don’t work very well, so stomach contractions are weak. Food just sits in the stomach for too long, delaying digestion and absorption of nutrients. One result is unpredictable blood sugar levels after meals, no matter how carefully you count carb grams. The medical term for these weak stomach contractions is gastroparesis.
From Diabetes Care:
“How is diabetic gastroparesis best managed?
Consultation by an RDN [registered dietitian, I reckon] knowledgeable in the management of gastroparesis is helpful in setting and maintaining treatment goals. Treatment goals include managing and reducing symptoms; correcting fluid, electrolyte, and nutritional deficiencies and glycemic imbalances; and addressing the precipitating cause(s) with appropriate drug therapy. Correcting hyperglycemia is one strategy for the management of gastroparesis, as acute hyperglycemia delays gastric emptying. Modification of food and beverage intake is the primary management strategy, especially among individuals with mild symptoms.
People with gastroparesis may find it helpful to eat small, frequent meals. Replacing solid food with a greater proportion of liquid calories to meet individualized nutrition requirements may be helpful because consuming solid food in large volumes is associated with longer gastric emptying times. Large meals can also decrease the lower esophageal sphincter pressure, which may cause gastric reflux [heartburn], providing further aggravation.
Results from a randomized controlled trial demonstrated eating plans that emphasize small-particle-size (<2 mm) foods may reduce severity of gastrointestinal symptoms. Small-particle-size food is defined as “food easy to mash with a fork into small particle size.” High-fiber foods, such as whole intact grains and foods with seeds, husks, stringy fibers, and membranes, should be excluded from the eating plan. Many of the foods typically recommended for people with diabetes, such as leafy green salads, raw vegetables, beans, and fresh fruits, and other food like fatty or tough meat, can be some of the most difficult foods for the gastroparetic stomach to grind and empty. Notably, the majority of nutrition therapy interventions for gastroparesis are based on the knowledge of the pathophysiology and clinical judgment rather than empirical research.”
Source: Nutrition Therapy for Adults With Diabetes or Prediabetes: A Consensus Report | Diabetes Care
Steve Parker, M.D.


![MP900385810[1]](https://diabeticmediterraneandiet.com/wp-content/uploads/2010/06/mp9003858101.jpg?w=214&h=300)

