Blood pressure control is also extremely important for protection of heart and kidneys
I’ve been reticent to tout the putative heart-protective effects of diabetes drugs in the classes called SGLT2 inhibitors and GLP-1 receptor agonists. Frankly, their supposed kidney-protective effects haven’t even been on my radar. My hesitation to report on these matters stems from:
Maybe if Big Pharma sent me a nice check….
The GLP-1 receptor agonists seem to have beneficial effects on both heart and kidney. With SGLT2 inhibitors, renal benefits may be more prominent than cardiac. Also note that any beneficial heart or renal effects may be attributable only to certain drug within the class, and not a class effect.
For what it’s worth, the American Diabetes Association recently hosted a conference on these issues. I assume the ADA endorses the report written by three experts, two of whom have received some sort of compensation from pharmaceutical companies. This doesn’t necessarily mean they are biased. Some excerpts:
Since patients with diabetes are at increased risk for CV [cardiovascular] and renal events, reducing the risk of these events is of primary interest to improve outcomes in the long-term. [Cardiovascular events usually refers to heart attacks, strokes, and death from those. Renal events would be high loss of protein through the kidneys, impaired kidney function or chronic kidney disease, or the need for dialysis.]
SGLT2 inhibitors and GLP-1 RAs have dramatically changed the treatment landscape of type 2 diabetes due to their established CV benefits, and the observed improvements in renal function seen with these classes of agents are currently undergoing intense investigation.
***
It is now apparent that both SGLT2 inhibitors and GLP-1 RAs show consistent reductions in major adverse cardiovascular events for patients with established cardiovascular (CV) disease, and both appear to have renal benefits as well.
***
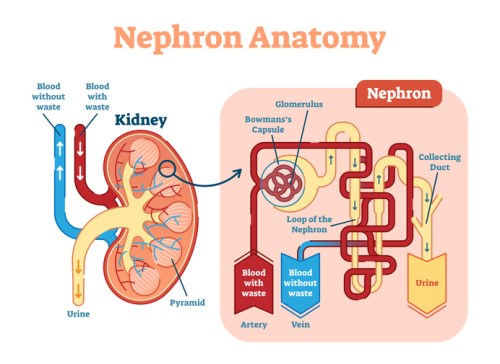
The nephron is the microscopic structural and functional unit of the kidney.
Renal effects of GLP-1 receptor agonists
These drugs may exert their beneficial actions on the kidneys through their effects on lowering blood glucose and blood pressure and by reducing the levels of insulin.
For GLP-1RAs, these [studies] include ELIXA with lixisenatide, LEADER with liraglutide, SUSTAIN-6 with semaglutide, EXCSEL with exenatide once-weekly, HARMONY with albiglutide, and REWIND with dulaglutide.
All these studies indicate that albuminuria [protein loss through urine] is reduced during treatment with GLP-1 RAs, and eGFR [estimated glomerular filtration rate, a measure of kidney function] appears to be stabilized.
These benefits are seen independently of HbA1c, weight, and blood pressure variations.
***
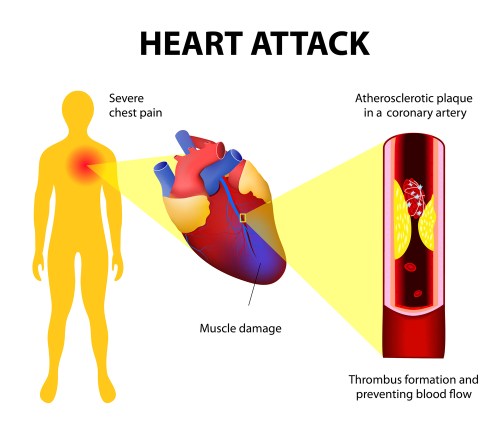
Heart attack is only one type of cardiovascular event
Cardiovascular effects of GLP-1 receptor agonists
Large CV outcomes trials with GLP-1 RAs have shown that these agents can reduce the risk of major adverse CV events, CV mortality, and all-cause mortality.
These CV benefits appear to be related to four distinct mechanisms:
-
- Improve myocardial [heart muscle] performance in ischemic heart failure [caused by poor blood flow to heart]
- Improve myocardial survival in ischemic heart disease
- Ameliorate endothelial dysfunction [endothelium is the lining of arteries]
- Decrease markers of CV risk.
***
Renal effects of SGLT2 inhibitors
- However, many potential mechanisms have been linked to the renoprotective effects of SGLT2 inhibitors.
- These include reduction of blood pressure, improved metabolic parameters, reduced volume overload, reduction in albuminuria, and glomerular pressure.
- For the latter, SGLT2 inhibition appears to reduce hyperfiltration via a tubuloglomerular feedback mechanism.
- Clinical data from CV outcomes trials have shown consistent variations in eGFR and reduction in death from renal causes with empagliflozin, canagliflozin, and dapagliflozin.
- However, to gain more information about the renal effects of these agents, dedicated renal outcomes trials are needed to study reductions in albuminuria, changes in eGFR, number of patients reaching end-stage renal disease, need for dialysis, and deaths due to kidney failure.
***
Key Messages from the authors
Large CV outcomes trials have shown that both SGLT2 inhibitors and GLP-1 RAs are associated with significant reductions in CV events in patients with elevated CV risk.
From CV outcomes trials both classes of agents also appear to have renal benefits, although large dedicated studies are needed to establish the magnitude of this potential benefit
The mechanism of action at the basis of CV and renal benefits of SGLT2 inhibitors and GLP-1 RAs is complex, multifactorial, and still not completely understood.
I’m still skeptical but will keep an open mind.
Steve Parker, M.D.
PS: Bold emphasis above is mine.

Click the pic to purchase at Amazon.com. E-book versions also available at Smashwords.com.